RESEARCH
April 2019
Hasan Ayaz1,2,3, Senior Member, IEEE, Kurtulus Izzetoglu1, Meltem Izzetoglu4, Banu Onaral1, Fellow, IEEE, Baruch Ben Dor5
1Drexel University, School of Biomedical Engineering, Science and Health Systems, Philadelphia, PA, 19104
2University of Pennsylvania, Department of Family and Community Health, Philadelphia, PA, 19104
3Children’s Hospital of Philadelphia, Center for Injury Research and Prevention, Philadelphia, PA, 19104
4Villanova University, Electrical and Computer Engineering, Villanova, PA, 19085
5Infrascan Inc, Philadelphia, PA, USA, 19104
Early identification of intracranial hematomas in patients with traumatic brain injury is crucial for the successful outcome of the intervention, specifically since expansion of the hemorrhage can result in debilitating and sometimes fatal outcomes. ‘Golden period’ refers to the time immediately following head trauma where assessment of the neurological condition and medical intervention of a victim is most needed and can significantly reduce the mortality and morbidity rate. Led by Britton Chance, we and an extended team from University of Pennsylvania, Baylor and Drexel Universities developed a handheld brain hematoma detector for early triage and diagnosis of head trauma victims. After obtaining De Novo FDA clearance, over two hundred systems were deployed in all United States Marine battalion aid stations around the world. The Infrascanner, a handheld brain hematoma detection system, is based on the differential near infrared light absorption of the injured vs. the non-injured part of brain. Twelve independent studies have been conducted in USA, Canada, Spain, Italy, Netherlands, Germany, Russia, Poland, India, China and Turkey with a total of 1293 patients and 203 hematomas [1]. Infrascanner demonstrated high sensitivity (adults: 92.5%, children: 93%) and specificity (adults: 82.9%, children: 86.5%) in detecting intracranial hematomas larger than 3.5 mL in volume and less than 2.5 cm from the surface of the brain[1]. The Infrascanner is a clinically effective screening solution for head trauma patients in pre-hospital settings where timely triage is critical.
Handheld medical device for hematoma detection
Every year an estimated 1.5 million Americans incur head injuries which represents only a fraction of the head injuries observed annually worldwide [2]. While there are many aspects of a head injury that must be addressed by a physician, the most urgent of these is brain bleeding or intracranial hematoma. Failure to detect and treat such injuries within the first several hours significantly increases the possibility of severe neurological deficits and even death [3, 4]. Patients with intracranial hematomas often require surgery, and therefore must be transported to a trauma center that has neurosurgical coverage. This requirement highlights the need for rapid and accurate initial screening for such injuries.
In rural and underdeveloped areas of the world as well as on a battlefield, timely identification of patients who require surgery can be difficult. Methods for identifying patients with hematomas in these settings primarily include a neurological exam and, when available, skull radiography. However, both of these modalities are notably unreliable[5-7]. The computed axial tomography (CT) scan is the gold standard for identification and localization of traumatic intracranial hematomas; however, its high cost and limited availability restricts its use in many areas of the world, and its high x-ray radiation poses risks for repeated scans and especially for children and pregnant women.
To address this need, Britton Chance from University of Pennsylvania and Claudia Robertson from Baylor College of Medicine developed a near infrared system for detection of brain hematomas and tested it successfully at Baylor. In collaboration with Drexel University team, a medical product was developed, obtained FDA clearance and tested successfully around the world. This collaborative effort resulted in Infrascanner, a handheld brain hematoma detection system that is based on the differential near infrared light (NIR) absorption of the injured versus the non-injured part of brain[8-11]. Under normal circumstances, the brain’s absorption can be assumed to be symmetrical. However, when additional underlying extravascular blood is present, there is a greater local concentration of hemoglobin. Consequently, the light absorbance is significantly greater and the reflected component is commensurately less. This differential is detectable via sources and detectors placed on symmetrical sides of the skull.

Figure 1. The Infrascanner 2000 handheld battery-operated sensor, front and back (left) disposable cap with light guides for NIR laser and detector positioned over scalp (middle) and, can be used at the site of injury (right).
Independent Clinical Studies
The Infrascanner development was supported initially by the Office of Naval Research and later by the Marine Corps System Command. So far, twelve studies have been published with 1,293 patients having over 200 hematomas as reviewed with meta-analysis in [1]. The studies were performed with diverse age populations and at different locations: USA, Canada, Spain, Italy, Netherlands, Russia, Poland, India, China and Turkey[12-24].
Real use case of the Infrascanner helping to save lives in Afghanistan
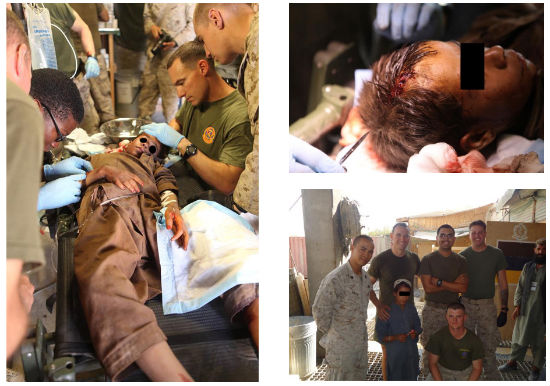
Infrascanner was introduced in Afghanistan in 2012 to address the need for a noninvasive and portable means of detecting intracranial hematoma. Intracranial hematomas are a treatable cause of secondary brain injury in patients who have sustained head trauma and have been reported to occur as the primary injury in 40% of patients with severe head injury. Successful treatment often relies upon diagnosis and intervention prior to neurological deterioration with CT examinations as the current clinical standard examination for detection of intracranial hematomas. However, serial CT is not practical or available in all cases and typically requires transport to a scanner. Using the Infrascanner in battlefield situations, the lives of a US serviceman and an Afghan boy were saved as the doctors were able to diagnose and treat severe head injuries before further complications arose.
In one case, an Afghan boy, who was at a scene of a suicide improvised explosive device (IED), was brought to the Marines doctor, who has the Infrascanner Model 2000 in Afghanistan. His examination showed a small laceration to his head. However due to a positive Infrascanner measurement he was evacuated to Kandahar. The examination there showed a skull fracture and frontal lobe hematoma. The boy was operated and did well after the surgery.
Figure 2. An Afghan boy, who was at a scene of a suicide IED, being examined by US Marines doctor. Bottom-right: Follow up photograph of the boy, together with the doctor who saved his life
Another real use case of the Infrascanner helping to save lives in Kenya
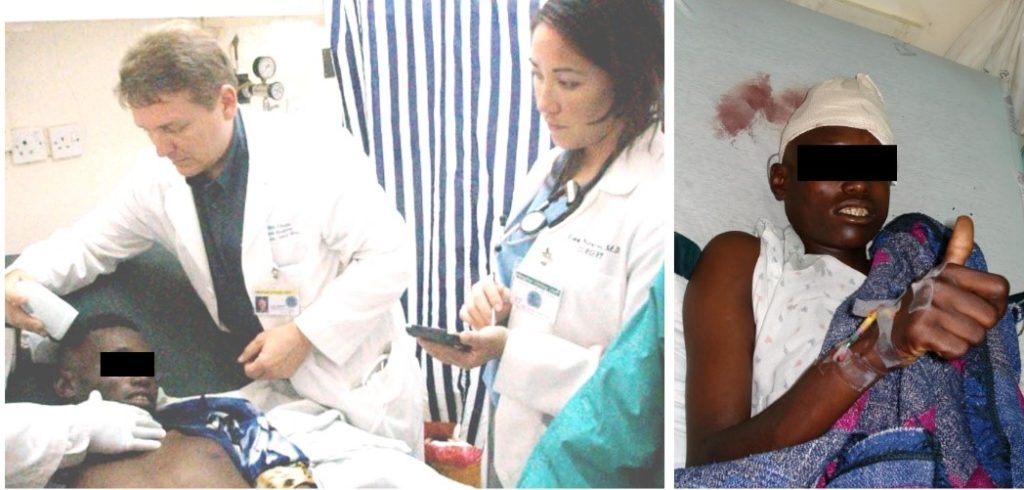
Another representative real use case of Infrascanner is from Tenwek, Kenya where nearest CT is 200 miles away in Nairobi. The patient, a 20ish male, fell off a truck with lucid interval and presentation 24hrs later with GCS 10. He had dilated left pupil and no speech. He was moving all extremities and with much purpose on the left. Dr. Mike Chupp applied Infrascanner and it was markedly positive for left frontal and temporal regions. The patient was taken into operation immediately and decompressed a huge epidural hematoma. The patient did well afterwards (see Figure 4) his thumbs up is using his right hand which is controlled by the saved left brain hemisphere.
Figure 3. During the initial assessment of the patient by Dr. Mike Chupp using Infrascanner (left), and the patient giving a thumbs up after surgery (right)
Conclusion
The Infrascanner is a clinically effective screening solution for head trauma patients in pre-hospital settings where timely triage is critical. It is intended to be used as an adjunct to the standard diagnostic workup to aid in the decision of choosing evacuation destination (a trauma center or the nearest hospital) and in prioritizing patients with suspected hematomas for urgent CT scans and surgical interventions.
NOTE: This article is informational and not an endorsement or recommendation of the IEEE Brain Initiative.
References
[1] H. Ayaz, M. Izzetoglu, K. Izzetoglu, B. Onaral, and B. Ben Dor, “Early diagnosis of traumatic intracranial hematomas,” Journal of Biomedical Optics, vol. 24, p. 10, 2019. [2] D. J. Thurman et al., Traumatic brain injury in the United States: A report to Congress. Centers for Disease Control and Prevention, 1999. [3] R. A. Cowley, “Trauma center. A new concept for the delivery of critical care,” The Journal of the Medical Society of New Jersey, vol. 74, no. 11, p. 979, 1977. [4] J. Melton, S. Jain, B. Kendrick, and S. Deo, “Helicopter Emergency Ambulance Service (HEAS) transfer: an analysis of trauma patient case-mix, injury severity and outcome,” Annals of The Royal College of Surgeons of England, vol. 89, no. 5, p. 513, 2007. [5] B. Jennett et al., “Severe head injuries in three countries,” Journal of Neurology, Neurosurgery & Psychiatry, vol. 40, no. 3, p. 291, 1977. [6] P. Perel, I. Roberts, O. Bouamra, M. Woodford, J. Mooney, and F. Lecky, “Intracranial bleeding in patients with traumatic brain injury: a prognostic study,” BMC emergency medicine, vol. 9, no. 1, p. 15, 2009. [7] S. C. Stein, C. Spettell, G. Young, and S. E. Ross, “Limitations of neurological assessment in mild head injury,” Brain Injury, vol. 7, no. 5, pp. 425-430, 1993. [8] S. Gopinath, C. Robertson, R. Grossman, and B. Chance, “Near-infrared spectroscopic localization of intracranial hematomas,” Journal of neurosurgery, vol. 79, no. 1, pp. 43-47, 1993. [9] H. Ayaz, B. Ben Dor, D. Solt, and B. Onaral, “Infrascanner: Cost Effective, Mobile Medical Imaging System for Detecting Hemotomas,” Journal of Medical Devices, Proceedings of Design of Medical Devices Conference, vol. 5, no. 2, p. 027540, 2011. [10] B. Onaral, H. Ayaz, M. Izzetoglu, K. Izzetoglu, D. Solt, and B. Ben Dor, “Update on a handheld brain hematoma detector project,” in Advanced Technology Applications for Combat Casualty Care (ATACCC), Fort Lauderdale, Florida, 2011. [11] C. S. Robertson, S. Gopinath, and B. Chance, “Use of near infrared spectroscopy to identify traumatic intracranial hemotomas,” Journal of biomedical optics, vol. 2, no. 1, pp. 31-42, 1997. [12] C.-y. Liang et al., “Chinese Military Evaluation of a Portable Near-Infrared Detector of Traumatic Intracranial Hematomas,” Military medicine, vol. 183, no. 7-8, pp. e318–e323, 2018. [13] L. Xu et al., “Portable near-infrared rapid detection of intracranial hemorrhage in Chinese population,” Journal of Clinical Neuroscience, vol. 40, pp. 136-146, 2017. [14] J. Peters, B. Van Wageningen, N. Hoogerwerf, and E. Tan, “Near-infrared spectroscopy: a promising prehospital tool for management of traumatic brain injury,” Prehospital and disaster medicine, vol. 32, no. 4, pp. 414-418, 2017. [15] Z. B. Semenova, A. Marshintsev, A. Melnikov, S. Meshcheryakov, A. Adayev, and V. Lukyanov, “Infrascanner™ in the diagnosis of intracranial lesions in children with traumatic brain injuries,” Brain injury, vol. 30, no. 1, pp. 18-22, 2016. [16] T. Braun, U. Kunz, C. Schulz, A. Lieber, and C. Willy, “Nahinfrarotspektroskopie zur Detektion intrakranieller traumatischer Hirnblutungen,” Der Unfallchirurg, journal article vol. 118, no. 8, pp. 693-700, August 01 2015. [17] G. Skotnicka-Klonowicz, J. Godziński, and A. Hermanowicz, “Management of minor to moderate head trauma in children–guidelines of the polish association of pediatric surgeons,” Standardy Medyczne/Problemy Chirurgii Dziecięcej., vol. 4, no. 1, pp. 42-50, 2014. [18] S. Bressan, M. Daverio, F. Martinolli, F. Mario, I. P. Steiner, and L. Da Dalt, “The use of handheld near-infrared device (Infrascanner) for detecting intracranial haemorrhages in children with minor head injury,” Child’s nervous system, vol. 30, no. 3, pp. 477-484, 2014. [19] R. Salonia, M. J. Bell, P. M. Kochanek, and R. P. Berger, “The utility of near infrared spectroscopy in detecting intracranial hemorrhage in children,” Journal of neurotrauma, vol. 29, no. 6, pp. 1047-1053, 2012. [20] C. S. Robertson et al., “Clinical evaluation of a portable near-infrared device for detection of traumatic intracranial hematomas,” Journal of neurotrauma, vol. 27, no. 9, pp. 1597-1604, 2010. [21] J. Leon-Carrion, J. M. Dominguez-Roldan, U. Leon-Dominguez, and F. Murillo-Cabezas, “The Infrascanner, a handheld device for screening in situ for the presence of brain haematomas,” Brain Injury, vol. 24, no. 10, pp. 1193-1201, 2010. [22] F. Coskun, E. A. Sezer, M. A. Karamercan, E. Akinci, and K. Vural, “An assessment on the use of infrascanner for the diagnosis of the brain hemotoma by using support vector machine,” Scientific Research and Essays, vol. 5, no. 14, pp. 1911-1915, 2010. [23] D. Lewartowska-Nyga, K. Nyga, and G. Skotnicka-Klonowicz, “Can infrascanner be useful in hospital emergency departments for diagnosing minor head injury in children?,” Developmental period medicine, vol. 21, no. 1, pp. 51-59, 2017. [24] B. Tyzo, T. Trojanowski, D. Szczepanek, and R. Rola, “Algorithm of initial management of mild head injury using the portable near-infrared spectroscope,” Neurol Praktyczna, vol. 2, pp. 13-20, 2014.
Biosketches
Hasan Ayaz (S’06–M’11–SM’18) is Associate Professor of Biomedical Engineering at Drexel University. Dr. Ayaz’s research involves understanding the neural mechanisms related to human perceptual, cognitive, and motor functioning with a focus on real-world contexts, utilizing mobile neuroimaging, and deploying neuroengineering approaches for neuroergonomics applications. His research aims to design, develop, and utilize (i.e. to measure->elucidate->enable) next generation optical brain imaging for neuroergonomic applications over a broad spectrum including aerospace to healthcare.
Kurtulus Izzetoglu, PhD is an Associate Research Professor of Biomedical Engineering at Drexel University, Philadelphia. His research and teaching interests are in functional brain imaging, human performance, learning, training, medical sensor development, biomedical systems and signal processing. He has background in both electrical and biomedical engineering coupled with experience of developing a highly portable functional near-infrared spectroscopy (fNIRS) system for use in field applications and translational neuroimaging. His recent research focusses on development of biosensors and biometrics for performance and training assessment, joint human-system performance enhancement for operational effectiveness, anesthesia and traumatic brain injury care monitoring in everyday practice.
Meltem Izzetoglu is an Associate Research Professor at Villanova University, Electrical and Computer Engineering, Villanova, PA. Dr. Izzetoglu’s research is centered around design, development and testing of functional Near Infrared Spectroscopy based brain imaging systems using laboratory phantoms, animal models and human experimentation, signal processing and algorithm development for artifact cancellation and biomarker extraction in biomedical applications specifically for cognitive activity assessment and physiological signal extraction in healthy, diseased and disabled populations of all ages.
Banu Onaral (S’76–M’78–SM’89–F’93) is H. H. Sun Professor of Biomedical Engineering and Electrical Engineering at Drexel University. She received her PhD in Biomedical Engineering from the University of Pennsylvania. Her research is centered on information engineering with special emphasis on complex systems and biomedical digital signal processing with emphasis on functional optical brain imaging. She has led major research and development projects and founded several laboratories including the CONQUER (Cognitive Neuroengineering and Quantitative Experimental Research) Collaborative.
Baruch Ben-Dor is the CEO of InfraScan. He received a Ph.D. in physics from the Technion and is a graduate of Talpiot program of the Israeli Air Force. He created InfraScan, a medical device company focused on handheld systems for detection of brain hematomas. He developed the company business plan, raised over $16M, got DeNovo FDA clearance and launched sales. All battalion aid stations of the US Marines are equipped with the Infrascanner, saving lives.